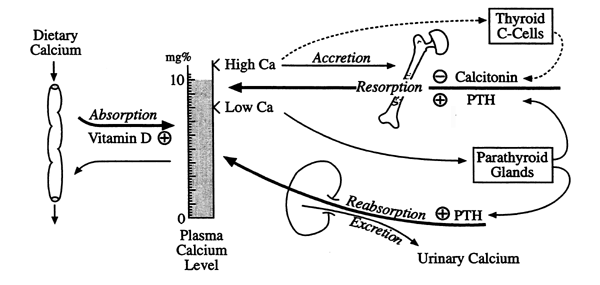
Calcium Homeostasis / PTH / Vitamin D
Physiology of Calcium, Phosphate and Bone:
99% of the body's Ca2+ is present in bones
1% is required for fertilization, vision, muscle contraction, nerve conduction, blood clotting, exocytosis, cell division and the activity of many enzymes and hormones
The concentration of calcium in the cellular and extracellular fluids must be maintained at a constant value.
Definitions:
Resorption: the process of breaking down and assimilating (Ca2+ mobilization)
Reabsorption: the process of re-absorbing (absorbing again)
1,25(OH)2D3: Vitamin D (active form, 1,25 D)
PTH: Parathyroid hormone
CT: Calcitonin
Physiology of Calcium Metabolism:

Low Plasma Calcium: stimulates PTH release, and PTH acts to resorb Ca2+ from the pool in bone and to enhance renal re-absorption of Ca2+
High Plasma Calcium: stimulates CT secretion which lowers plasma calcium by inhibiting bone resorption
Parathyroid Hormone:
i) functions to raise plasma calcium via bone resorption and renal calcium reabsorption
ii) stimulates the metabolism of Vitamin D to its active hormonal form, 1,25(OH)2D3
Parathyroid Hormone Secretion and Calcium Homeostasis in the Parathyroid Cell:
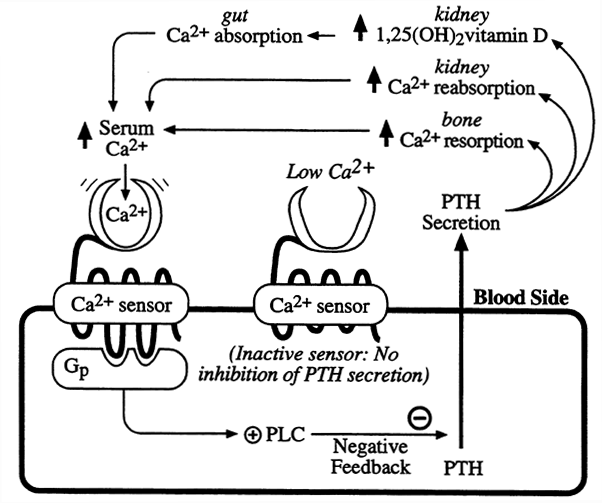
1,25(OH)2D3: enhances PO43- and Ca2+ absorption which in turn eleicits bone mineralization preventing Rickets in children and bone remodeling / strengthening in adults
Vitamin D: more later.....
Functions-
i) promotes calcium absorption from the gut
ii) promotes calcium reabsorption from the kidney
iii) promotes calcium mobilization from bone via resorption
iv) enhances phosphate absorption by the intestine
Control of Blood Ca2+ and PO43-:
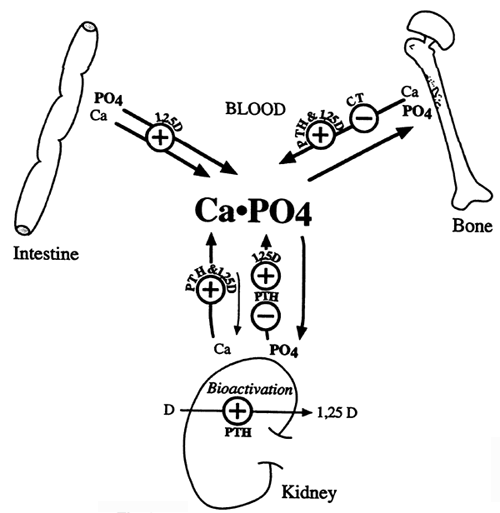
Clinical Correlate(s):
Hyperparathyroidism-
Excessive PTH usually due to a Parathyroid Adenoma, breaks the feedback loops
Symptoms- renal stones, bone pain (due to increased bone resorption)
Hypoparathyroidism-
Lack of PTH (usually due to removal of the parathyroid gland along w/ the thyroid)
Symptoms- hypocalcemia
Treatment- large doses of 1,25(OH)2D3 to raise blood calcium through intestinal calcium absorption
Parathyroid Hormone (PTH): Chemistry, Biosynthesis and Biochemical Actions
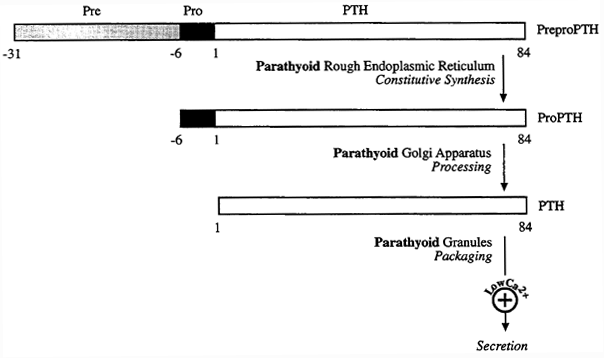
PTH is an 84 A.A. peptide initially biosynthesized as prepro-PTH
PTH acts upon target cells primarily to increase cAMP via Gs
Kidney is the primary site of PTH action
PTH infusion will sharply increase urinary cAMP levels, as well as producing a marked increase in urinary phosphate levels (PTH inhibits renal phosphate reabsorption)
Clinical Correlate: Pseudohypoparathroidism (PsHP)
Symptoms: short stature, round face, abnormally short fingers and toes, subcutaneous calcification and mental deficiency
Cause: deficiency in the Gs protein that couples receptors to adenylate cyclase, Gs activity is only about 50% of normal
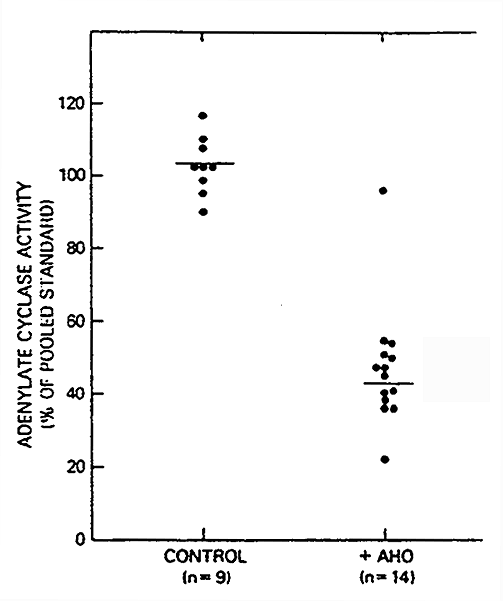
Since Gs couples many other hormone receptors to adenylate cyclase, TSH, glucagon etc, severely affected patients display resistance to these hormones as well.
Calcitonin (CT): is a 32 amino acid peptide secreted by the thyroid under conditions of hypercalcemia
It operates via receptors in bone that are coupled to adenylate cyclase through Gs and raise cAMP levels.
How can CT act on bone to lower Ca2+ resorption while PTH increases resorption when both function via Gs to raise cAMP???
Answer: two opposing hormones can act via the same signal transduction pathway in the same tissue if they affect different cell types.
CT raises cAMP in bone resorbing osteoclasts ----> inhibit their activity
PTH raises cAMP in osteoblasts ----> secrete resorptive factors ----> activate osteoclasts
Vitamin D:
The Synthesis of Vitamin D:
Vitamin D is classified as a fat soluble vitamin, however with adequate sunlight exposure humans do not need dietary vitamin D because with sunlight vitamin D can be synthesized from 7-dehydrocholesterol
Photosynthesis of Vitamin D3:
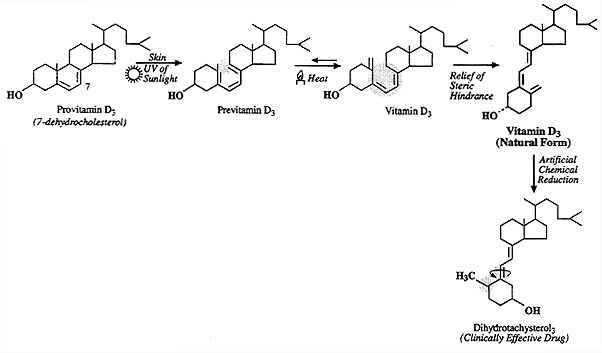
Metabolism of Vitamin D:
Vitamin D itself does not act upon intestine, kidney and bone but must be bioactivated in the liver and kidney
The Bioactivation and Inactivation of Vitamin D3:
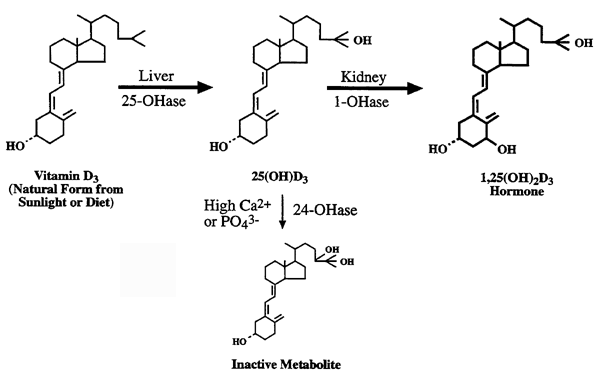
1. It stimulates calcium absorption more rapidly than other forms of vitamin D.
2. It is more active on a molar basis than any other form.
3. it is produced in kidney in a regulated fashion, based on the need for calcium and/or phosphate.
4. It has specific receptors in intestine, bone and kidney.
5. It chemically resembles the steroid hormones.
Regulation of 1,25(OH)2D3 Production:
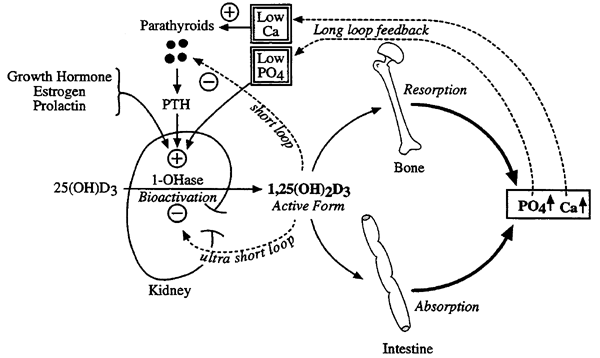
OHase- Hydroxylase
Note: When Ca2+, PO43- and 1,25(OH)2D3 are elevated, 25(OH)D3 is metabolized to 24,25(OH)2D3 an inactive metabolite.
1,25(OH)2D3 production is stimulated under the following conditions:
1. Low dietary calcium: PTH is secreted, which activates the 1-OHase in kidney to produce 1,25(OH)2D3.
2. Low dietary phosphate: direct enhancement of kidney 1-OHase.
3. Active growth in children: via growth hormone stimulation of 1-OHase.
4. Pregnancy and lactation: estrogens and prolactin increase renal 1,25(OH)2D3 output.
Biochemical Mode of 1,25(OH)2D3 Action:
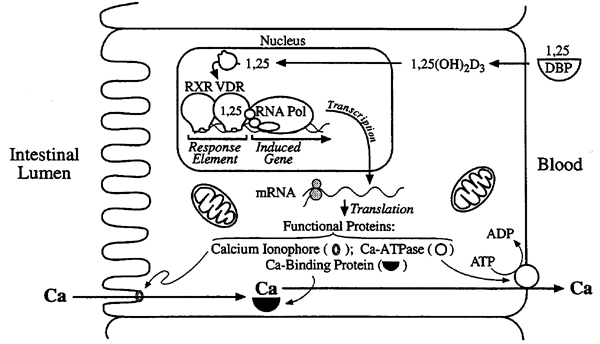
The proposed mode of action for 1,25(OH)2D3 resembles the mode of action of the general class of thyroid/steroid hormones:
i) transport to nucleus
ii) mediation by a nuclear receptor
iii) stimulation of DNA transcription
iv) synthesis of functional proteins: Calcium Transporter (Ionophore), Ca-Binding Protein and Ca-ATPase.
Clinical Correlate(s):
Rickets- "a disease marked by soft deformed bones caused by vitamin D deficiency"
Type I:
Symptoms- delayed walking, severe rickets
Serum Chemistry- low Ca2+, high PTH and phosphate, high 25(OH)D3, low 1,25(OH)2D3
Cause- defective 1-OHase enzyme in kidney
Treatment- physiologic replacement doses of 1,25(OH)2D3
Type II:
Symptoms- rickets, bowing of lower extremities, hair loss
Serum Chemistry- low Ca2+, high PTH, normal 25(OH)D3 and elevated 1,25(OH)2D3
Cause- target tissue resistance to 1,25(OH)2D3, receptor or post-receptor defect
Treatment- mega doses of 1,25(OH)2D3
Osteoporosis:
Symptoms-clinically significant loss of bone mass resulting in fractures of the vertebrae, wrist or hip
. Affects over 27 million individuals in the U.S. and about 1.5 million fractures are . attributable to osteoporosis annually in people 45 and older.
. Of those women who live to age 90, 32% will suffer hip fracture.
. Cost of oteoporosis is $10 billion annually.
Prevention- adequate dietary calcium plus vitamin D, regular exercise, estrogen replacement for post-menopausal women.
© Dr. Noel Sturm 2019